Persistent Corneal Epithelial Defects: Casey Hogan, OD, FAAO, FSLS
Background
A 53-year-old Caucasian female was referred by a local corneal specialist for a scleral lens fitting for a Persistent Corneal Epithelial Defect (PCED). Her chief complaint at time of examination was that of moderate redness with associated blurred vision of her left eye. She presented under the assumption she was wearing a soft bandage contact lens (BCL) OS prescribed by the referring doctor that provided minimal relief. This case report will demonstrate the successful use of scleral lens therapy in the management of PCED as a complication of scleral buckle retinal detachment repair surgery, pars plana vitrectomy (PPV), and endolaser.
Test Procedures, Fitting/Refitting, Design, and Ordering
Visit #1: Initial Visit
Unaided Distance Visual Acuity
OD: 20/20
OS: 20/100 (PHNI)
Pupils were unequal with a fixed surgical mydriatic left pupil. No afferent pupillary defect was noted by reverse pupil testing. Confrontation fields and ocular motility testing were full OU. iCare tonometry readings were normal OU.
Anterior and Posterior Segment Examination
Clear lids and lashes OU. The conjunctiva was white and quiet OD, but grade 1+ hyperemia was present OS. The cornea was clear OD, but evaluation of the cornea OS revealed a 2 mm x 2 mm epithelial defect with no associated infiltrate. Microcystic epithelial edema was present OS. No BCL was detected. No associated anterior chamber reaction was present OS. Irises were flat and blue OU. The lens was clear OD. A posterior chamber intraocular implant was present OS with grade 2 posterior subcapsular opacification. Dilated fundus examination was deferred secondary to recent examination by the treating retinologist and reported as stable OU.
Treatment Plan
The 8.4 Plano Acuvue Oasys BCL OS was replaced. Slit lamp examination revealed adequate BCL centration and movement. Topical moxifloxacin 0.5% ophthalmic solution was prescribed one drop four times daily OS. Copious non-preserved artificial tears were recommended. The patient was scheduled to return for re-evaluation and scleral lens fitting with the goal to stabilize the PCED.
Visit #2: Scleral Lens Fitting Visit
Slit Lamp Biomicroscopy
Minimal conjunctival hyperemia and mild microcystic epithelial were present OS. The BCL was present and carefully removed. Trace fluorescein epithelial punctate stain was present with resolution of the frank defect. Given near complete resolution of the defect, refractive analysis and corneal topography were performed.
Manifest Refraction
OD: -0.25 -0.50 x105 (20/20)
OS: Plano (20/30)
Corneal Topography

Diagnostic Lens Selection
The Blanchard MSD mini-scleral lens design was selected for this patient due to ease of handling. Based on the patient’s HVID of 13.1 mm OS and average palpebral fissure width of 10 mm, a 15.8 mm overall diameter (OAD) was selected over the 18.0 mm OAD.
The initial diagnostic lens sagittal depth value determination was 4.40. This was determined by evaluating the corneal/scleral profile. Blanchard’s MSD fitting guide recommends starting with the 4.40 for patients with moderate KCN, PMD, keratoglobus, as well as in the case of keratometric readings between 42.00 and 45.00. This patient’s central keratometric readings were flatter at 39.00 @13/40.99 @103; however, based on the corneal topography and corneal profile, and the consideration of a healing epithelial defect, we did not want to risk any corneal touch with the initial lens choice. A sagittal depth value of 4.40 was determined to be the best initial starting point.
The next parameter selected was the profile curve, which provides the most appropriate vault for the limbal zone area. A standard (S) profile was selected based on corneal topography. Although use of corneal topography to determine the base curve of standard small diameter corneal gas permeable lenses is routine, in the fitting of scleral lenses evaluation of the overall corneal topographic map to determine the degree of irregularity and analysis of the elevation maps is helpful in selecting the best initial lens.
Finally, the “standard” scleral edge zone value was selected for proper alignment in hopes to provide an adequate landing that would minimize lens seal off, conjunctival impingement, or lens edge stand-off. The diagnostic lens was filled with non-preserved sterile saline with a small amount of fluorescein dye, and applied utilizing a large DMV tool. The patient was comfortable and assured during the application process.
Initial Diagnostic Lens
Blanchard MSD Select/15.8 OAD/Sagittal Depth Value 4.40/ S Peripheral Profile /Standard lens edge/CT 300 microns/-2.00D
The lens was evaluated after approximately five minutes of settling time. Excessive apical clearance (approximately 500 µm) was present indicating that the vault was too steep. The lens was removed. In order to reduce the clearance, the sagittal depth value was reduced and the new lens selected had a sagittal depth value equal to 4.20.
Second Diagnostic Lens
Blanchard MSD Select/15.8 OAD/Sagittal Depth Value 4.20/ S Peripheral Profile /Standard lens edge/CT 300 microns/-2.00D.
The lens was evaluated and revealed approximately 300 µm of apical clearance via comparing the post lens tear layer to the center thickness of the diagnostic lens (300 µm). The lens provided adequate limbal clearance and good scleral landing without impingement nor stand-off. The patient noted good comfort.
The lens was allowed to settle for one hour and Zeiss anterior segment optical coherence topography (AS-OCT) was utilized to evaluate the fit utilizing the caliper function. Central clearance was measured to be 240 m µm (Figure 2) and the post lens tear layer was clear of significant debris. Final lens power was determined by over-refraction with visual acuity equal to 20/20-2 and trial lens to demonstrate quality of vision to the patient. The patient was very pleased with the comfort and the vision.

Final Lens Order
Blanchard MSD Select/15.8 OAD/4.20 Sagittal depth/S profile/Standard Edge/-1.75 DS power/Boston XO2 material
Patient Consultation and Education
Visit #3: Dispense Appointment
Slit Lamp Biomicroscopy
The BCL was in place and removed with jeweler’s forceps. The epithelium was intact and trace punctate linear stain was present OS. Minimal conjunctival hyperemia was present OS. It was determined to be safe to proceed with the scleral dispense appointment.
Scleral Lens Evaluation
The new ordered lens was filled with preservative-free saline solution and a small amount of fluorescein dye and inserted utilizing a large DMV. The patient immediately reported good comfort and vision. Thirty minutes was allowed for settling of the lens. Visual Acuity was 20/20 OS with plano over-refraction.
Slit lamp examination revealed adequate apical and limbal clearance OS. The lens was centered with proper coverage and edge alignment. A small amount of fluorescein dye was applied to the superior and inferior bulbar area to evaluate for any tear exchange or toricity. No visible fluorescein was visible in the post lens tear layer after five minutes.
AS OCT revealed central clearance to be equal to 262 µm (Figure 3).

Application, Removal, and Care Education
The patient was educated on proper scleral lens application utilizing the large DMV and removal utilizing the small DMV, with emphasis on the proper DMV application location. The patient demonstrated proficiency with her application and removal technique. Care products prescribed included peroxide-based solution for disinfection, non-preserved inhalation saline 3mL vials with non-preserved Oasis Tears for insertion, and Oasis Tears for pre/post wear of the lens. Personal hygiene and hand washing were emphasized. The typical scleral lens wear schedule prescribed is four hours plus two each day up to a maximum of twelve hours; however, given the lens was aimed at reducing the recurrence of the epithelial defect, full daily wear was recommended. The patient was instructed to remove the lens and return to clinic immediately if any pain, excessive redness, or blurred vision was noted.
Follow-up Care and Final Outcome
Visit #4: Two Week Follow-Up
The patient returned to clinic for her two-week follow-up examination of her left scleral lens. She reported wearing the lens six hours at time of presentation. The patient reported doing very well. No redness or blurred vision was reported. The patient was extremely happy and reported being able to wear the lens all day. Proper care and lens schedule was reviewed, and the patient reported compliance with all recommendations.
Entering acuity with the MSD lens was 20/20 OS. Slit lamp examination revealed good centration, adequate apical clearance, limbal clearance, and edge alignment. Minimal microcystic edema was present in the area of the original defect. AS OCT revealed apical clearance equal to 205 µm (Figure 4). Limbal vault was equal to 54 and 58 µm respectively. Minimal lens impingement was noted OS. The patient was instructed to return for her one month follow-up.

Visit #5: One Month Follow-Up
At the one-month follow-up visit, the patient reported doing very well with good vision and minimal redness noted OS. Entering visual acuity was equal to 20/20-2 OS. Slit lamp examination revealed a well-fitting lens with only mild lens edge impingement noted. AS OCT was not performed on this visit. The cornea was stable with no epithelial defected noted. No lens parameter changes were ordered at this time. The patient was scheduled to return to clinic in three months and to return immediately if any redness or reduced vision noted.
Visit #6: Three Month Follow-Up
At the three-month follow-up visit, the patient reported good vision, but mild redness of the nasal corner of the left eye. Overall, the patient was very happy and reported compliance with lens care. Entering acuity was 20/20 OS. Slit lamp examination revealed adequate apical and limbal clearance. Mild lens edge impingement was noted with trace nasal conjunctival hyperemia and very light blanching 360 degrees. AS OCT was performed at this point revealing a central vault of 206 µm. The edge landing was adequate; however, given the mild nasal hyperemia and blanching 360 degrees a new lens was ordered with a 1 FLAT edge profile. Given the dynamics of the edge and vault relationship, to compensate for the reduced vault from a flat edge design, a 4.30 sagittal depth and power parameter change to -1.25DS were ordered. The patient returned for the dispense of the new lens a week later. The edge landing was improved 360 degrees and adequate apical clearance was noted with the 4.30 sagittal depth.
Recent Follow-Up (Three Years after Initial Fitting)
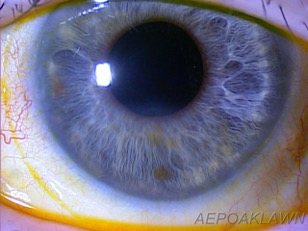
The patient has been doing very well with scleral lens therapy for treatment of her PCED OS. No recurrence of the epithelial defect has been noted for nearly three years now. Visual acuity OS with the lens was equal to 20/20-2 O. Slit lamp examination revealed a stable ocular surface and optimal scleral lens fitting (Figure 5). The patient continues to see her corneal specialist biannually with no new treatments recommended.
Discussion/Alternative Management Options
In review of the literature, there are few case reports that discuss PCED after retinal surgery and pars plana vitrectomy. HF Chen et al. reviewed the incidence, risk factors, and clinical course of PCED after pars plana vitrectomy5. They concluded that the overall incidence of PCED after PPV was equal to 4.8% (n=511 eyes), and PCED after PPV were correlated with poor postoperative outcomes, and because of this, aggressive management was recommended. The patient presented in this case report was originally treated by her corneal specialist, and despite aggressive management with standard therapies, the outcome was poor. Scleral lens therapy in the management of this patient was considered and ultimately led to success.
Standard management of PCED typically includes the use of copious lubrication, discontinuation of topical medications that may be iatrogenic, punctal occlusion, debridement, soft bandage contact lenses, amniotic membrane patching or grafting, autologous serum, tarsorrhaphy, or more recently the use of scleral lenses have emerged. After a complete PubMed literature review, the treatment of PCED unresponsive to standard therapies with a scleral lens was first reported by Rosenthal P. et al.6. Extended wear of a fluid-ventilated gas permeable scleral contact lens was reported. This retrospective study involved fourteen eyes (n=14) of thirteen patients who had failed to heal with traditional therapies. Success in healing of the epithelial defects was seen in eight of the fourteen patients. An important consideration is that four of the fourteen treated eyes developed microbial keratitis.
In 2013, Lim P. et al. demonstrated efficacy in the use of the Boston Scleral Lens, known as PROSE (Prosthetic Replacement of the Ocular Surface Ecosystem), in the treatment of PCED7. Continuous wear of PROSE with concomitant moxifloxacin antibiotic therapy in the reservoir was employed in 20 eyes of 19 patients (n=19). Re-epithelialization occurred in 17/20 eyes. This retrospective interventional case series reported no cases of microbial keratitis. The addition of the topical preservative-free moxifloxacin to the PROSE reservoir likely was instrumental in reducing the risk of microbial keratitis. In 2015, Ciralsky et al. showed in a retrospective review of 8 eyes that continuous wear of a PROSE device, using a strictly standardized regimen, constitutes an effective, safe treatment option for refractory persistent epithelial defects. No microbial keratitis was reported8.
Another noteworthy strategy is to consider the concomitant use of topical autologous serum tears and scleral lenses in the treatment of PCED. The efficacy and safety of topical 100% serum drops for post-surgical corneal epithelial defects has been reported by Lekhanont et al.This study reported a 93.92% success rate in the treatment of 178/181 patients who received 100% topical autologous serum eye drops. The median time to complete re-epithelization was 4 days9. Huang W, et al. Studied the use of autologous serum drops for treating PCED after vitreoretinal surgery. Although the study number was only equal to three patients, all patients healed with autologous serum therapy within two weeks after other strategies failed, and the use of autologous serum has now become standard care by the authors in any vitreoretinal surgical patient that develops PCED10. The concomitant use of scleral lenses and serum tears for the treatment of PCED needs further study.
In summary, this case report demonstrates that scleral lens therapy can be very successful in the management of post-surgical PCED. It is always important for clinicians to determine the etiology of the PCED prior to treatment. Scleral lens therapy should be considered as a treatment option after other standard therapies have failed. This case demonstrated daily wear scleral therapy versus extended wear. More recent studies have shown extended wear therapy to be effective in promoting re-epithelialization; however, careful measures should be taken to prevent microbial keratitis. The future of scleral lenses in the management of many forms of ocular surface disease is promising, and certainly deserves continued study.
References
- Katzman L, Jeng B. Strategies for persistent epithelial defects of the cornea. Saudi Journal of Ophthalmology. 2014.28:168-172.
- Delmonte D, Kim T. Anatomy & Physiology of the Cornea. J Refract Corneal Surg. 2011. 37:588-598.
- Dahlgren MA et al. Persistent epithelial defects. In: Albert DM, Miller JW, eds. Albert & Jakobiec’s Principles and Practice of Ophthalmology. Philadelphia: Elsevier; 2008:749-759.
- Schornack M, et al. Scleral Lenses in the Management of Ocular Surface Disease. Ophthalmology 2014;121(7):1398-1405.
- Chen H, et al. Persistent Corneal Epithelial Defect Pars Plana Vitrectomy. Retina 2016;36(1):148-155.
- Rosenthal, P et al. Treatment of persistent corneal epithelial defect with extended wear of a fluid-ventilated gas-permeable scleral contact lens. American Journal of Ophthalmology 2000;130(1):33-41.
- Lim, P et al. Treatment of Persistent Corneal Epithelial Defect with Overnight Wear of a Prosthetic Device for the Ocular Surface. American Journal of Ophthalmology 2013;156(6):1095-1101.
- Ciralsky, B et al. Treatment of Refractory Persistent Corneal Epithelial Defects: A Standardized Approach Using Continuous Wear PROSE Therapy. Ocul Immunol Inflamm. 2015;23(3):219-24.
- Lekhanont K et al. Topical 100% Serum Eye Drops for Treating Corneal Epithelial Defect after Ocular Surgery. BioMed Research International, vol. 2013, Article ID 521315, 7 pages, 2013.
- Huang WC, Chiang CC, Tsai YY. Autologous serum eye drops for treating persistent corneal epithelial defect after vitreoretinal surgery. Cornea 2008;27(9):1097.
Back to Table of Contents
